6 results
First psychotic episode due to inmunosupresor medication
- A. Corrales, L. Unzue, L. Llovera, N. Cancelo
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1047
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
48-year-old man from Spain who lived with his wife until he got divorced 4 months before starting the follow up in Mental Health. The debut was in September 2021 with a hospitalization in the Brief-acute hospitalization unit due to florid psychotic clinic-
He consumed several drugs in his twenties (cocaine, marihuana and heroin IV) and was diagnosed of HIV at the age of 29. He abandoned the use of drugs after the diagnoses and keep good adherence to the antiretroviral treatment (Abacavir + Lamivudine +Efavirenz).
At the age of 46 (January 2020), he was successfully transplanted a kidney. Afterwards, he started taking inmunosupresor medication to avoid transplant rejection
At the few months of the transplant and the beginning of the inmusosupresor medication, the patient became more irascible with moments of remarkable disinhibition and progressive abandon of the work obligations.
In January of 2021, he got divorced after months of difficulties with his wife, married 28 years before, due to the mentioned problems as well as moments of bizarre and disorganized conducts and suspicion towards his wife with probable delusional jealousy. He, therefore, lost his job, hose and marriage and started taking drugs again after 17 years of abstinence.
He was hospitalized in e Brief Acute Inpatient Unit in September 2021 with distrustful and hypervigilant attitude- He was suffering from delusional ideation of harm and persecution with high distress and emotional repercussion. He also presented disorganized conduct and probable auditory hallucinations. He was positive to amphetamines and cocaine After 3 days without consuming; there was no remission of the clinic.
ObjectivesDiscussing the association between the initiation of inmunsupresor medication and the beggining of psychotic clinic
MethodsFirst psychotic episode (FEP) has a likely consequence of the initiation and maintenance of Tacrolimus -due to a kidney transplant- with the concomitant abuse of amphetamines and cocaine as a trigger factor.
The psychotic clinic progressively remitted in one week after the administration of 3 mg/day of risperidone.
The antiretroviral treatment was changed due to the poor adherence during the disorganization period. The tacrolimus was not removed because of the good response to the neuroleptic and the risk of transplant rejection
ResultsThe patient started with prodromic symptoms of psychosis at the time he began with the inmunosupresor medication. Progresively, the psychotic clinic worsen wit the consequence of a biographical break with the consequence of a divorce, therlost of work and home and a drug relapse.
ConclusionsThere is evidence of the association between psychotic episodes in people with no psychiatric history and the inmunosupresor medication for the kidney transplant (Above all, tracolimus). This case remarks the need of an exhaustive medical anamnesis in the diagnosis of psychiatric pathologies.
Disclosure of InterestNone Declared
Non-convulsive epiletic seizure after electroconvulsive therapy session
- L. Llovera García, L. Veiga Gil, L. Lopez Unzue, A. Corrales Rodriguez, A. Ballesteros Prados, J. Yoldi Murillo, J. M. Lopez Ilundain
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1021-S1022
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Electroconvulsive therapy (ECT) is a procedure performed under general anaesthesia involving triggering an intentional brief seizure through small electrical currents through the brain. The anaesthetic depth should be adequate prior to shock and measured with BIS, a processed electroencephalogram (EEG) monitor. Adjusting the hypnotic dose allows to decrease the ictal threshold and thus improve the response to treatment and decrease side effects.
ObjectivesOur goal is detecting elements such as spontaneous epileptiform activity after ECT without tonic-clonic activity with the spectral density matrix (SDM).
MethodsOur patient: an 87-year-old woman, diagnosed with F20.2 catatonic schizophrenia and under antipsychotic treatment since her youth. She has required multiple hospital admissions due to psychopathological decompensations until starting monthly maintenance ECT sessions in 2014. Since then she no new hospital admissions have been required.
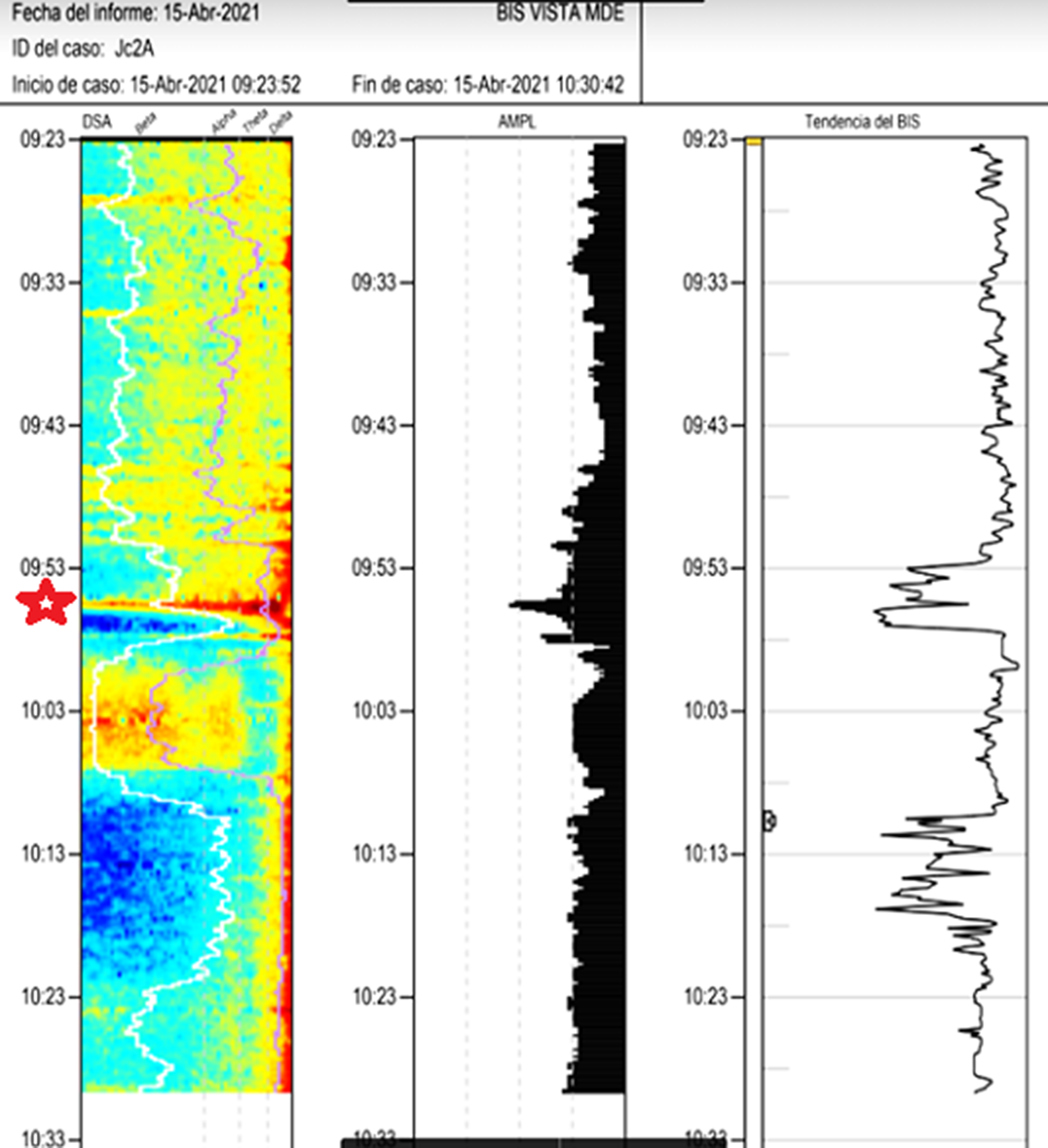
ResultsImages 1D and 1E shows the SDM, a spectrogram of the EEG. The X axis show time (minutes), the Y axis shows the frequency (Hz) and the Z axis shows the energy or intensity of that electrical activity in the frequency bands replaced by colors: warm colors (red) reflecting high intensity electroencephalographic activity and cool colors (yellow, blue and green), low activity. Images 2 and 3’s EDM shows spontaneous epileptiform activity after electroconvulsive therapy without tonic-clonic activity. We observed an initial EDM of an awake patient, with warm colours in practically all frequency bands, including the beta band (13-30 Hz), characteristic of waking states. Around 9:50 anaesthetic induction occurs, activity increases in slow frequencies (red colours in alpha, theta and delta), plus an increase of cold colours in beta, reflecting the disappearance of brain activity in that frequency. The asterisk reflects the EEG response to the electrical discharge, followed by a postcritical state with brain activity exclusively in slow waves and high amplitude (delta and some theta) and absence of activity in other frequencies (blue colour in the beta and alpha bands) around 9:57. At about 10:00 there is an abrupt appearance of high intensity brain activity (warm colours) in beta and alpha and delta, mainly, reflecting spontaneous epileptiform activity after treatment and clinically reflected as a patient absent and disconnected from the environment, but without tonic-clonic activity. New postcritical state in which blue colour predominates, reflecting little brain activity, and warmer colours reappear in all frequency bands, including beta, reflecting the progressive recovery of wakefulness.
Image:
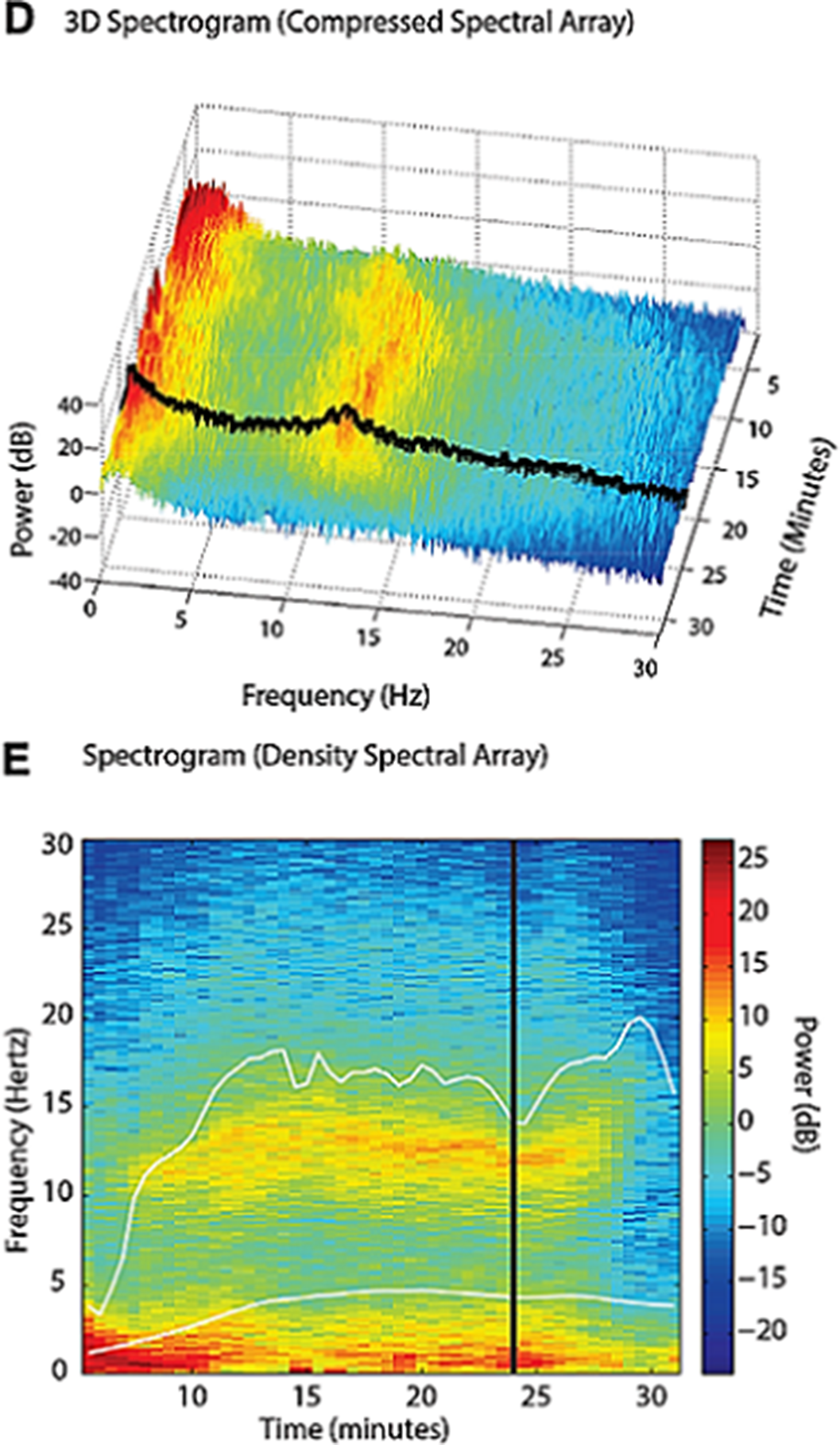
Image 2:
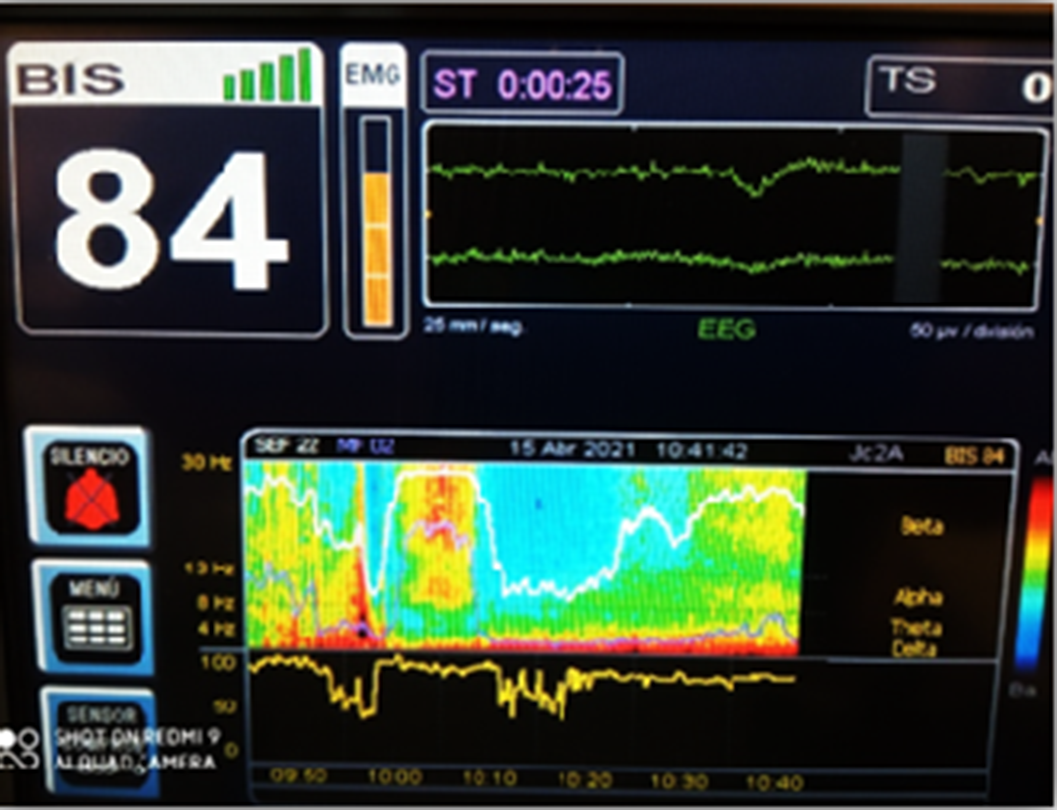
Image 3:
 Conclusions
ConclusionsPsychiatric pathology can be reflected in the SDM, which allows to observe changes in the EEG, correcting the electrical stimulus of the shock and the dose of anesthetic appropriate to the patient to trigger an intentional brief seizure under general anesthesia.
Disclosure of InterestNone Declared
¿What do we know about Very Early Onset Schizophrenia? - A case report
- L. Unzue, J. Royo, L. Llovera, A. Corrales
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S728
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
This is a case aboout a 12-year-old girl, lives with her mother, father and younger brother. Parents originally from Peru, the patient was born in Spain.
She started follow-up by Mental Health in May 2022 due to low self-esteem after school bullying. The parents report that she has always been a shy child with many insecurities; she has always been insecure and suspicious in her relationships with peers, but during the last school year she was more nervous and insecure with everything that had happened to her; this situation was the reason for requesting a consultation at an Infant-Juvenile Mental Health Center when the school year was about to end.
In October she went to the emergency department accompanied by her parents because she seemed different in the last few days. A few days ago, while the patient was returning on the school bus, the patient began to write to her mother commenting that her classmates were imitating her, and that she noticed strangers not only in her classmates but also in her teachers, and in her own parents, thinking that they were imitating her. She had not slept well for several days.
In the interview alone with the patient, she was distrustful, hypervigilant, referring that the therapists were imitating her. She verbalized delusional ideation of harm and auditory hallucinations with high distress and emotional repercussions. She also presented slightly disorganized speech and formal thought disorders. In the last few days she had also been aggressive towards her younger brother and mother.
She had presented a febrile condition two weeks ago that subsided with antibiotics.
As a family history, she has a father’s aunt diagnosed with paranoid schizophrenia.
ObjectivesDue to the seriousness of the situation and the impossibility of performing an outpatient approach, it was decided to perform an urgent admission to the Infanto-Juvenile Brief Inpatient Unit with the objectives of performing a diagnostic affiliation, organic screening and evolutionary follow-up.
MethodsDue to the febrile picture that had presented two weeks ago, and the recent onset of symptomatology, it was decided to request the following tests: abdominal ultrasound, cranial MRI and electroencephalogram. All tests were normal.
ResultsDue to the normality of the complementary tests requested, it was diagnosed as F29 Non-organic psychosis without specification. Treatment with Risperidone was started.
ConclusionsTwo months later, the patient has had a good evolution, but still continues to present psychotic symptoms, such as auditory hallucinations and delusional ideation of harm, but with less impact than at the beginning.
The evolution of the case points to a possible diagnosis of Schizophreniform Disorder, due to the persistence of psychotic symptoms, less than 6 months after the debut.
Due to the age of the patient, we would be facing a diagnosis of VEOS (Very Early Onset Schizophrenia).
Disclosure of InterestNone Declared
Results of the Employment-Activity Program (EAP) of the PEPsNA in patients with first-episode psychosis
- L. Aranguren, A. Aquerreta Unzue, M.C. Ariz Cia, L. Azcarate Jimenez, A. Fernandez Falces
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S771-S772
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The Employment-Activity Program (EAP) of the PEPsNA aims that people develop or regain the occupational roles to wich ther aspire in their life after a first episode, due to the early ages affected by psychosis. Social-labor integration strategies (vocational rehabilitation and supported employment) are effective tools to improve the evolution of people with serious mental illnes.
ObjectivesCheck the objectives achieved by the PEA, which in turn serves as a self-assessment, in order to improve our daily work.
MethodsData related to employment/occupation are analyzed, (number of people who are active in employment or carrying out standarized studies, people with temporary labor disability or who repeat a year, sheltered employment, occupational center, long-term unemployment and others), instrumental functional capacity and neurocognitive status (CGI COG scale), occupational disability (WHODAS scale), social and occupational functioning (SOFAS scale) and quality of life (QLS scale)
ResultsThe rate of active persons with employment or standarized studies increases by 7.2% at 24 months, and the long-term unemployment rate decreases by 4.9%, the timing of the highest occupation being at 12-18 months of treatment, reaching 55% and the one with the lowest unemployment at 12 months, with 17.3%. The percentage of people with ILT falls by 13.4%. The functioning scales also detect an improvement after 2 years of treatment.
ConclusionsThe PEA contributes to the improvement in the global funtioning of people and their quality of life.
DisclosureNo significant relationships.
Homeostasis Model Assessment of IR (HOMA-IR) and Metabolic Syndrome (MetS) in First Episode Psychosis
- E. Garcia De Jalon, L. Aranguren Conde, A. Aquerreta Unzue, G. Gutiérrez Talavera, A. Corrales Rodriguez
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S769
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Metabolic syndrome (MetS) is common in chronic psychosis but also exists in the early stages. HOMA-IR is an independent predictor of cardiovascular diseases and has already been described in first episode of psychosis.
ObjectivesTo determine whether HOMA levels differ according to MetS at each time assessment over 2 years.
MethodsMetS and HOMA levels are determined at baseline and at 6, 12, 18 and 24 months in a sample of 50 patients participating in the PEPsNa Early Intervention Programme during two years of follow-up. Adult Treatment Panel III (ATP III) criteria are used to define MetS. Insulin resistance measured with the Homeostatic Model Assessment (HOMA-IR) is computed with the formula fasting plasma glucose (mg/dL) times fasting insulin (mIU/mL) divided by 405. Mann-Whitney U Test are used to compare HOMA variable according to presence of metabolic syndrome.
ResultsThe results showed that HOMA levels differed statistically significantly between patients who met MetS criteria and those who did not at 12 (p<0.046) and 24 (p<0.004) months of treatment.
ConclusionsGiven the small sample size the results of our study indicate that there is a sustained relationship over time between HOMA levels and Metabolic Syndrome (MetS) and that the HOMA IR may be useful in identifying those patients with an increased metabolic and cardiovascular risk.
DisclosureNo significant relationships.
Course of the Metabolic Syndrome (Mets) in a First Episode Psychosis Sample
- E. Garcia De Jalon, L. Aranguren, A. Fernandez Falces, A. Aquerreta Unzue, N. Pereda
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S247-S248
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is evidence that metabolic syndrome (MetS) is common in chronic psychosis but also exists in the early stages.
ObjectivesTo study the prevalence and course of MetS over a period of 2 year after a first episode psychosis. To determine whether there may be differences in its prevalence according to the type of antipsychotic used over two years.
MethodsA sample of 300 patients participate in the PEPsNa Early Intervention Programme. SMet was determined at baseline and at 6, 12, 18 and 24 months. The type of antipsychotic used at each assessment moment is collected (none, aripiprazole, paliperidone, others). Adult Treatment Panel III (ATP III) criteria were used to define MetS.
ResultsThe prevalence of MetS at baseline is 4.44% and increases to 7.96% at 6 months, 10.1% at 12 months, 8.62% at 18 months and 9.01% at 24 months. The prevalence of MetS increases at 6 (p<0.021) and 12 months (p<0.003) compared to baseline and then remains stable. Only at 6 months assessment there are significant differences (F-Ficher p<0.022) in the presence of MetS (15.8%) in the paliperidone group treatment (oral or LAI).
ConclusionsMetabolic syndrome (MetS) exists from the early stages of psychosis and increases in the first 6-12 months and remains stable thereafter. The type of antipsychotic treatment only seems to have an influence at 6 months, with no differences at other follow-up times.
DisclosureNo significant relationships.






